
If you’ve ever been curious about the ins and outs of working with a home birth midwife, this one’s for you! Today, we’ll hear from Shelly Schedler of Sacred Journey Midwifery in Cleveland, Ohio, and learn how she got into midwifery, her approach, and much more. Read on to learn more about Shelly.
How long have you been a home birth midwife and what got you into midwifery?
I started my midwifery apprenticeship and school at the National College of Midwifery in late 2020 and graduated as a CPM (certified professional midwife) at the end of 2023. I’ve been a birth doula since 2008 and have known for many years that I would eventually become a home birth midwife. Birth work draws me with its raw beauty and the unique way it requires anyone entering that space to step into a place of intuition and, quite often, surrender and humbleness.
My birth partner, Staci Dasher (also a CPM), and I work together to serve families in Cleveland and Northeast Ohio. I have an office in my home in Wickliffe, I see people at my partner’s home office in Novelty, and I have access to an office in Jefferson, Ohio.

What’s your favorite thing about being a home birth midwife?
I love building relationships with the families we serve. I love the provider/client trust built within the midwifery model of care. More than anything, I love seeing people come into the inherent power that pregnancy and birth bring about.
Can you walk me through a typical home birth, from the initial consultation to the postpartum follow-up?
Our clients typically meet with us for a consultation, where any questions they have about home birth and our services can be discussed. Staci and I share what brought us into midwifery and our philosophies on pregnancy, birth, and postpartum.
When we are chosen as someone’s midwifery team, we have around 12 prenatal appointments (depending on if we start care at the beginning of pregnancy) where we assess and record vitals, listen to and count the baby’s heartbeat, measure uterine growth, conduct urinalysis, discuss nutrition, troubleshoot any issues, share information, and just provide encouragement for the childbearing journey.
When a mother enters the time that her baby can safely be born at home, we are officially on call for that family until the birth. Our goal is to arrive quietly at a birth when mom is in active labor and assess how labor is progressing. After we make sure the immediate needs of mom/family are taken care of, we then take and record vitals, intermittently listen to the baby’s heart rate, evaluate how contractions may be affecting him/her, and remain ready to help mom with any strategies that might either progress labor or promote a proper rest and adequate energy levels.

Once baby is born, while mom (and family) and baby are getting their first glimpses of each other, one of us stays keenly aware of how mom is doing while the other focuses on how the baby is doing. We love the golden hour where bonding occurs and honor and respect that space.
After a birth, (if help is needed) we assist with getting baby latched to the breast, make any necessary repairs to mom’s perineum, help her get into fresh clothes, clean the space up, give parting instructions, tuck mom and baby and partner into bed, and quietly exit.
We come back in 24 hours to observe for normalcy in the heart, lungs, appearance, and behavior of the newborn and for normalcy in the postpartum healing process for mom. We are back between 3-5 days (sometimes 7 days), 14 days, and 6 weeks postpartum to assess both mom and baby. During all of this time, we stay in contact, inquiring about any concerns that may be developing, and when necessary we refer our clients to additional healthcare professionals.
How do you work with families to create a birth plan that fits their needs and preferences?
An important part of my work as a home birth midwife is spending lots of time discussing and learning about what a family’s desired birth plan might look like in the prenatal timeframe. We spend time envisioning what the birth space might look like and encourage clients to do the same.
What would you say to someone with a concern or fear about home birth?
I would tell them that our culture likes to impart the fearful/risky nature of almost everything we do, and it teaches us to trust something or someone outside of ourselves more than our intuition and instinct. This is not a good balance. It’s up to us to find our way back to our inner beings so that we can decide where we belong and how to let go of our culturally programmed fears. Only then can we know where we truly need to be when giving birth.
I think there is a normal fear that comes with giving birth. Along with that are excitement, power, and beauty. When we think only in terms of fear we sometimes forget about the other feelings and emotions. It’s all about balance.
What are some unique or innovative techniques you use as a home birth midwife to ensure a safe and comfortable experience for the mother and baby?
Starting in pregnancy we like to teach families that when labor starts there is a rhythm that needs to be respected that consists of rest, nutrition, and movement.
When we get to a house where a mom is in labor we mostly try to stay out of the way unless we’re needed. Labor knows how to happen on its own, our bodies know how to give birth, and babies are great at dancing their way into being born.
Sometimes, though, help is needed. When that occurs, we love using body mechanics and positional techniques to help babies shift into more optimal positions. Forward leaning inversion, side lying release, asymmetrical leg lunging, deep knees/chest, hands and knees, counter pressure, double hip press—anything to give the pelvis variation in its position so that the baby can engage the way he/she needs to.
Also, if a mom is getting exhausted, we encourage nutrition and rest. We stress the importance of making sure mom is going to the bathroom enough because if the bladder is full that can make contractions ineffective.
It really is all about what is happening in the moment and what our client’s individual needs are.
How do you help families prepare for the possibility of transfer to a hospital during a home birth? In what circumstances do you decide it’s time to transfer to the hospital?
We discuss what circumstances may warrant a transfer during our prenatal appointments. We talk about how that might make our clients feel. We have a simple form that is filled out in case of both emergent and non-emergent transfer which indicates at a glance: mom’s blood type, preferred hospital (both in emergency and non-emergency situations), phone number of the preferred labor unit, preferred pediatrician, and any other pertinent information. We also assure our clients that at least one of us will accompany them to the hospital if a transfer occurs.
Can you talk about the role of the father or partner in birth? How do you support them in their role?
Dads can be great sources of comfort for laboring moms. There is an intense and intimate interaction that occurs between couples when both are involved in the labor and birth process. We teach partners how to help with positional techniques, counter pressure, how to help keep mom hydrated and nourished, how to respect the birth space, and also that rest and nutrition are essential for partners as well.

How do you incorporate evidence-based care into your home birth midwife practice? What resources do you use to stay current on the latest research?
CPMs are required by the North American Registry of Midwives (NARM) to get 30 continuing education units every 3 years. Beyond that, I personally love to research the current information available about any topics that arise and dig up studies that pertain to issues we are seeing. I use the National Institutes of Health (NIH), the Cochrane Database, midwifery textbooks, and other midwives to keep my understanding fresh and current.
Can you discuss any cultural considerations you take into account when working with families from diverse backgrounds?
I welcome families from all different backgrounds including different religions, ethnicities, and sexual orientations. If someone has a need or a background that I am not familiar with, I am willing to learn and/or refer them to someone who might serve them better.
Do you have any tips for families who are considering a home birth?
If you know what you want, ask all the questions you can! If you are not sure what you’re looking for in a midwife, reach out to other people who have had a home birth and ask them for tips.
Some examples of topics that people tend to care deeply about:
- Under what conditions will your midwife transfer your care to another provider during pregnancy and/or birth?
- Is the home birth midwife willing to be as hands-on or hands-off as you need them to be?
- Does the home birth midwife align with your philosophies about birth?
- Is the midwife trained in neonatal resuscitation and CPR?
- How was your midwife trained? Apprenticeship? How long)? School? Which one? Both?
- Is your home birth midwife certified through NARM?
- Does someone on the birth team accompany you to the hospital if there is a transfer during labor?
Ultimately, you will want to feel safe in your midwife’s presence. You really want to gauge how you feel during your interview. Excited? Nervous? Comfortable? Connected? Tense? Unsure? Pay attention to these feelings and use them to make your decision as well.
What are some common misconceptions about home birth that you would like to address?
Some people think that if a person is not tolerant of pain, they are not a good candidate for a homebirth. Birth is hard work and very intense; it is also painful at times. However, it is a normal physiological process that our bodies have built-in capabilities to do. Pain tolerance for being injured may not be the best barometer for pain tolerance in labor. We are capable of so very much.
How do you handle emergencies during a home birth?
When there is an emergency during a home birth, Staci and I first let the parents know what is happening. If there is a decision to be made by the parents we give them space to do that, otherwise, we get to work performing our tasks (i.e. resuscitation; stimulation; calling EMS, helping parents prepare for the hospital). We decide who will go to the hospital with the parents and the other person stays back to clean. At times we have both gone to the hospital and both gone back to the house to clean. It all depends on the situation and the client.
How do you work with families to ensure they have a positive birth experience, regardless of the outcome?
We often discuss the what-ifs of hospital transfer during pregnancy so that our clients are at least open to the possibility. It is difficult for all who are involved in a home birth when the decision is made to transport. I think that both parents and midwives tend to second guess their actions/non-actions and try to come up with solutions that might work better moving forward, even if nothing could have prevented the transfer. I think it’s ok for parents to spend some time reflecting and grieving if their plans for a home birth did not come to fruition.
One thing that I think makes everything smoother and more positive is knowing any hospital staff who might have some sensitivity toward the family/mom who needs to transfer. The more our surrounding hospital staff and home birth midwives become collaborative instead of suspicious of one another, the safer our home birth parents will feel when they do need to transfer.
How do you ensure continuity of care for families during the postpartum period?
Our team—myself and my birth partner Staci—continue to care for clients during the postpartum time. We see our clients 24 hours after their births, 3-5 days, (sometimes 7 days), 14 days, and 6 weeks. Many times we are in contact with those families multiple times in the weeks and months after their births.

How, if at all, do you work with other healthcare providers (OBs, pediatricians, etc.) to ensure the best care for families?
We have a running list of pediatricians in the surrounding areas who our clients tell us are positive towards home-birthing families. We always remember the hospital staff who made our transfers feel friendly and safer. Staci and I both attended a meeting at Suma of Akron in which doctors, nurses, and midwives all got together to determine how to make transfers smoother and better for home birth clients. We hope to have the opportunity to meet with other local hospital staff in the future to discuss transfer care and best practices for our home birth families.
Can you talk about any specific training or qualifications you have that make you well-suited to assist with home births?
In 2008, I began my journey as a birthworker as a certified birth doula through Childbirth International. I’ve been attending both hospital births and home births since then. I began two midwifery apprenticeships in early 2021. I now have an Associate of Science in Midwifery from the National College of Midwifery and earned the North American Registry of Midwives (NARM) CPM credential in late 2023.
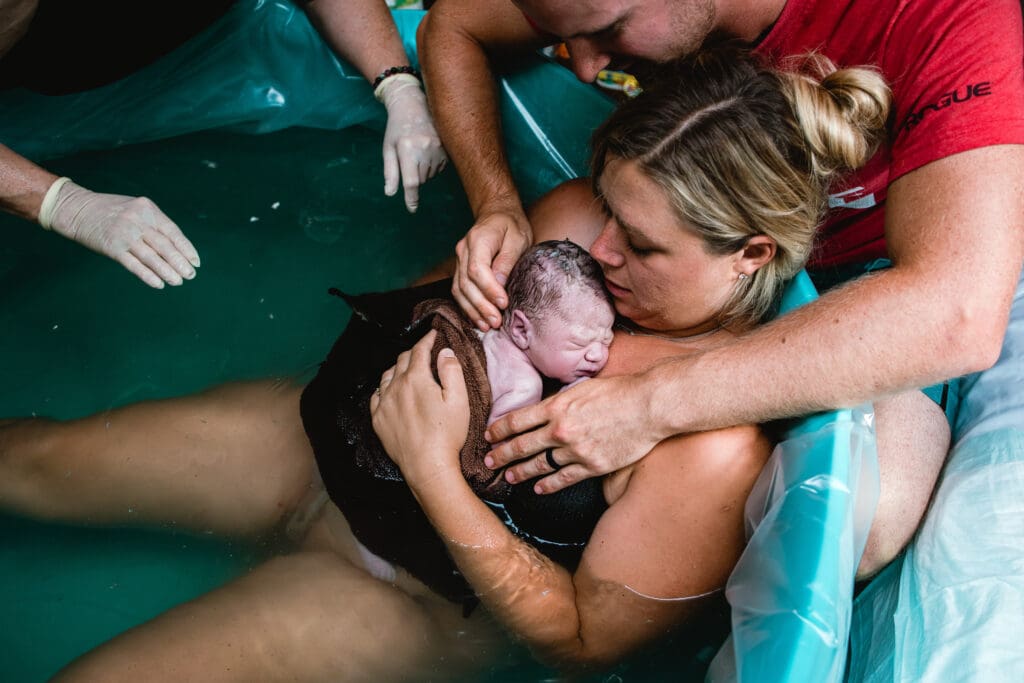
Can you share any experiences you’ve had with water birth and how it can benefit the mother and baby during labor and delivery?
I would estimate that around 50% – 60% of the births I have attended have been water births. In my experience as both a doula and home birth midwife, I’ve witnessed firsthand how water can relax a laboring mother, which is amazing and essential right around active labor, transition, and pushing.
Studies show that water therapy during labor and birth can cut down on the length of labor, decrease the need for medicated pain relief, increase relaxation hormones, decrease damage to perineal and vaginal tissues, decrease estimated blood loss, increase infant-maternal bonding, and all without increasing complications or negative neonatal outcomes.
Something else that is very compelling about the topic of water birth can be found in this position paper by the International Childbirth Education Association, which has shown the GBS transmission rate for water births is lower—1 in 4432—than that of land births, which is 1 in 1450. I would love to see more studies that focus on this!

Can you share any examples of how you have supported families who have had a previous traumatic birth experience and how they were able to have a positive birth experience?
When someone has had a previous traumatic birth experience, I try to talk through that experience in bite-sized chunks over the course of their pregnancy, as that mom and family are able. It’s important to me to be sensitive to actions and attitudes that could be triggering to those who have suffered birth trauma and to always send the message that a pregnant and birthing mom has autonomy and agency over her situation.
What pregnancy or birth-related resources do you always recommend to people?
Mother Rising’s Birth Circle in Chardon, Ohio is a great in-person resource for local families.
I also love Lily Nichols’s book, Real Food for Pregnancy and Birthing From Within by Pam England and Rob Horowitz.
Is there anything else you’d like to share about yourself?
I love hiking, backpacking, coffee, my Great Pyrenees (Brynn), and spending time with my adult children and my grandson. Being a midwife is a dream that has come to fruition (I’ve known for over 20 years that I wanted to do this). It is a great honor to serve families as a homebirth midwife.
Where can people connect with you to learn more about what you offer?
You can reach out to me via my Facebook page, Sacred Journey Midwifery Services, or send me an email at shellbellsched@gmail.com.
I also have a new Facebook group called (Home)Birth Matters of Lake County, Ohio.
I hope you enjoyed reading and learning more about Shelly and the world of being a home birth midwife. It’s a unique and empowering experience that can be a reality with the right support!
Click here to connect with Cleveland home birth midwife Shelly Schedler.

Hey there and thank you for stopping by! I’m Mackenzie, owner of Mackenzie Romagni Photography, a birth, newborn, and family photographer serving growing families in Cleveland and Northeast Ohio. I hope you found this “Meet a Midwife: Home Birth Midwife Shelly Schedler of Sacred Journey Midwifery” blog post helpful.
Are you expecting a new baby and hoping to hire a birth photographer for your hospital, birth center, or home birth? Contact me here to connect! Not quite ready yet? No problem! Follow me on Instagram or join my email list here to stay in the know.

+ Comments